Patients with Chronic Limb-Threatening Ischemia (CLTI)
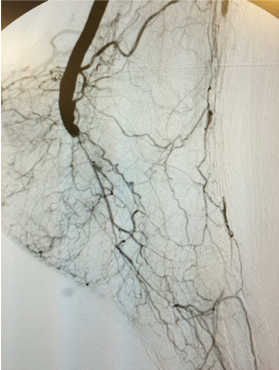
Condition
The incidence of peripheral artery disease (PAD) has increased over the years due to population aging and the global epidemic of diabetes. Some patients progress to chronic limb-threatening ischemia, an advanced stage of PAD. Chronic limb-threatening ischemia (CLTI) is associated with increased mortality, risk of amputation, and impaired quality of life. CLTI is a clinical syndrome defined by the presence of PAD in combination with rest pain, gangrene, or a lower limb ulceration >2 weeks duration.
The recent Global Vascular Guidelines (GVG) have focused on defining, evaluating, and managing CLTI with the goals of improving evidence-based care, patient outcomes and identifying critical research needs. Vascular surgeons are your partners in caring for your patients with CLTI with a shared goal to improve limb salvage, survival and maximize quality of life.
When to Refer
All patients with suspected CLTI should be referred urgently to a vascular surgeon for limb salvage efforts. All patients with rest pain, non-healing foot ulcers/wounds, or gangrene should have vascular testing to assess blood supply and potential for healing.
Why Refer to a Vascular Surgeon
Vascular surgeons are experts in selecting and interpreting appropriate hemodynamic tests and imaging studies for the diagnosis and management of CLTI. They will also collaborate with you to optimize your patient’s cardiovascular health, including managing their risk factors and reinforcing the importance of smoking cessation.
Vascular surgery is the only discipline among the American Board of Medical Specialties which has specific training requirements to study the natural history and medical treatments of CLTI. Vascular surgeons are the only specialists who can perform all therapies (medical, minimally invasive, endovascular, and open surgeries) for CLTI. A vascular surgeon can be your partner to help you and your patients get the most comprehensive management of their vascular disorder as well as the treatment that is best for them. Early referral and collaboration with a vascular surgeon can lead to better outcomes for each patient.
Evidence-Based Guidelines
CLTI: Useful Evidence-Based Guidelines for Referring Physicians
“Chronic limb-threatening ischemia (CLTI) is a clinical syndrome defined by the presence of peripheral artery disease (PAD) in combination with rest pain, gangrene, or a lower limb ulceration >2 weeks duration. CLTI is associated with amputation, increased mortality and impaired quality of life. . . . All patients with suspected CLTI should be referred urgently to a vascular specialist.”
All patients with rest pain, non-healing foot ulcers/wounds, or gangrene should have vascular testing to assess blood supply and potential for healing. Vascular surgeons are experts in selecting and interpreting appropriate hemodynamic tests and imaging studies for diagnosis and management of CLTI.
| Recommendation | Grade | Level of Evidence | Key References |
1.1 Definitions and nomenclature
| 1.1 |
Use objective hemodynamic |
1 (Strong) | C (Low) | de Graaff16 2003 Brownrigg17 2016 Wang18 2016 |
Early referral to a vascular surgeon for limb salvage efforts is recommended.
| 6. Strategies for EBR |
| 6.1 | Refer all patients with suspected CLTI to a vascular specialist for consideration of limb salvage, unless major amputation is considered medically urgent. | Good practice statement |
| 6.19 | Do not classify a CLTI patient as being unsuitable for revascularization without review of adequate-quality imaging studies and clinical evaluation by a qualified vascular specialist. | Good practice statement |
7.6 |
Do not offer HBOT to improve limb salvage in CLTI patients with severe, uncorrected ischemia (e.g., WIfI ischemia grade 2/3). | 1 (Strong) | B (Moderate) | Kranke1102015 Game1112016 Santema1122018 |
Medical management of patients with CLTI and PAD is an important aspect of their care. You and your vascular surgeon will work as a team to optimize your patient’s cardiovascular health, including managing their risk factors and reinforcing the importance of smoking cessation.
| 4. Medical Management |
| 4.1 | Evaluate cardiovascular risk factors in all patients with suspected CLTI. | 1 (Strong) | B (Moderate) | I.C.A.I. Group301997 |
| 4.2 | Manage all modifiable risk factors to recommended levels in all patients with suspected CLTI. | 1 (Strong) | B (Moderate) | Armstrong31 2014 Faglia32 2014 |
| 4.3 | Treat all patients with CLTI with an antiplatelet agent. | 1 (Strong) | A (High) | Antithrombotic Trialists’ Collaboration332002 Antithrombotic Trialists’ Collaboration342009 |
| 4.4 | Consider clopidogrel as the single antiplatelet agent of choice in patients with CLTI. | 2 (Weak) | B (Moderate) | CAPRIE35 1996 Hiatt36 2017 |
| 4.12 | Offer smoking cessation interventions (pharmacotherapy, counseling, or behavior modification therapy) to all patients with CLTI who smoke or use tobacco products | 1 (Strong) | A (High) | Dagenais582005 Athyros59 2013 Blomster602016 |
| 4.13 | Ask all CLTI patients who are smokers or former smokers about status of tobacco use at every visit. | 1 (Strong) | A (High) | Kondo61 2011 Newhall62 2017 |
Longitudinal care of a patient with CLTI after limb salvage or amputation is essential and should be coordinated between referring providers and vascular surgeons.
| 10. Postprocedural care and surveillance after infrainguinal revascularization for CLTI |
| 10.1 | Continue best medical therapy for PAD, including the long-term use of antiplatelet and statin therapies, in all patients who have undergone lower extremity revascularization. | 1 (Strong) | A (High | Abbruzzese1252004 Henke1262004 Brown1272008 Bedenis1282015 Suckow1292015 |
| 10.2 | Promote smoking cessation in all CLTI patients who have undergone lower extremity revascularization | 1 (Strong) | A (High | Hobbs130 2003 Willigendael1312005 |
| 10.3 | Consider DAPT (aspirin plus clopidogrel) in patients who have undergone infrainguinal prosthetic bypass for CLTI for a period of 6 to 24 months to maintain graft patency. | 2 (Weak) | B (Moderate) | Brown,27 2008 Belch132 2010 Gassman133 2014 Bedenis128 2015 |
| 10.4 | Consider DAPT (aspirin plus clopidogrel) in patients who have undergone infrainguinal endovascular interventions for CLTI for a period of at least 1 month. | 2 (Weak) | C (Low) | Cassar134 2005 Bhatt135 2006 Tepe136 2012 Strobl137 2013 |
| 10.14 | Provide mechanical offloading as a primary component for care of all CLTI patients with pedal wounds. | 1 (Strong) | A (High | Elraiyah143 2016 |
| 10.15 | Provide counseling on continued protection of the healed wound and foot to include appropriate shoes, insoles, and monitoring of inflammation. | 1 (Strong) | A (High | Elraiyah143 2016 |
Reference:
Global vascular guidelines on the management of chronic limb-threatening ischemia
Michael S. Conte, MD (Co-Editor), Andrew W. Bradbury, MD (Co-Editor), Philippe Kolh, MD (Co-Editor), John V. White, MD (Steering Committee), Florian Dick, MD (Steering Committee), Robert Fitridge, MBBS (Steering Committee), Joseph L. Mills, MD (Steering Committee), Jean-Baptiste Ricco, MD (Steering Committee), Kalkunte R. Suresh, MD (Steering Committee), M. Hassan Murad, MD, MPH
Joint guidelines of the Society for Vascular Surgery, European Society for Vascular Surgery, and World Federation of Vascular Societies
Endorsed by the American Podiatric Medical Association, British Cardiovascular Society, British Society for Endovascular Therapy, British Society of Interventional Radiology, Circulation Foundation, College of Podiatry, Society of Interventional Radiology, Society for Vascular Nursing, the Society for Vascular Technology of Great Britain and Ireland, and the Vascular Society of Great Britain and Ireland.
J Vasc Surg 2019:69:3S-125S
https://doi.org/10.1016/j.jvs.2019.02.016