Vasculitis refers to a group of disorders that involve inflammation of blood vessels. The inflammation is due to the immune system attacking and damaging your arteries, veins and/or capillaries.
Uncommon
About 1–2 new cases of vasculitis per 50,000 people are found each year. Vasculitis affects men and women of all ages and races.
Can Be Episodic or Last a Lifetime
The duration of vasculitis ranges from short-term to lifelong. Patients often have episodes or flares over a period of years.
Infographic by National Heart Lung and Blood Institute (NIH) [Public domain], via Wikimedia Commons
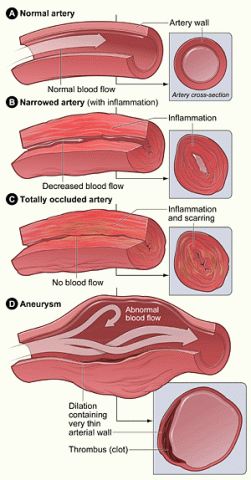
Vasculitis can affect a wide range of organs in your body. Therefore, symptoms vary depending on where the condition develops. However, vasculitis remains a systemic disease. Generalized symptoms such as fatigue and non-specific pain, and side effects of medications used in the treatment of vasculitis often present a challenge.
The most common symptoms include:
- Fever
- Generalized pain/headaches
- Fatigue
- Shortness of breath/cough (if your lungs are involved)
- Skin rashes/spots
- Numbness or pain in a hand or foot
Some forms of vasculitis affect your kidneys. This may result in no symptoms at all.
The causes of vasculitis are largely unknown. Vasculitis disorders are classified as autoimmune diseases. This means that by mistake your immune system attacks itself for unknown reasons. There is evidence that both genetic factors (inheritance) and environmental factors play a role. Environmental factors that have been linked to vasculitis include some long-term infections (bacteria, viruses or fungi) and medications that cause a “hyperactive” allergic immune response.
See a Vascular Surgeon
Diagnosis often starts with your doctor suspecting you may have vasculitis based on symptoms and a physical exam. If this is the case, see a vascular surgeon. You will be asked questions about symptoms and medical history, including questions about family members. The vascular surgeon will also perform a physical exam.
Tests Help Refine the Diagnosis
Many tests can help determine the type of vasculitis (small-, medium- or large-vessel disease). The most common tests are:
- Blood tests that can detect the presence of inflammation and identify some proteins in the blood that are commonly found in vasculitis patients. ESR (erythrocyte sedimentation rate) and CRP (C-reactive protein) tests both help detect the presence of inflammation in the body. The ANCA (antineutrophil cytoplasmic antibodies) test looks for proteins commonly found with vasculitis disorders.
- A biopsy is the removal of a small sample of tissue that bears signs of being affected by vasculitis for examination under a microscope. This is often the best way to diagnose the disease.
- Imaging tests can also be helpful. Options include X-rays to look at blood vessels while injecting a dye into the bloodstream to identify patterns/narrowing of vessels (angiography); MRI (Magnetic Resonance Imaging); and CT (Computed Tomography) scans.
Treatment of vasculitis is aimed at suppressing parts of the immune system and reducing inflammation. In more severe cases, treatment focuses on reducing disability that may be caused by the disease and preventing damage to vital organs.
Medication can be used to suppress parts of the immune system.
- Glucocorticoids, often known as steroids, (like prednisone, prednisolone) and other immunosuppressants, also called cytotoxic medicines, (like methotrexate, cylciphosphamide) are the most frequently prescribed drugs to treat vasculitis. The dosage and duration of treatment depends on disease type and severity.
- Newer immunosuppressant drugs, such as rituximab, have been found to be effective against certain types of vasculitis.
Other Therapies
- Plasmapheresis (blood filtration to remove certain proteins) and intravenous immunoglobulin (specific type of antibody) have also been used to treat the disease.
- Angioplasty, a minimally invasive procedure, is helpful when vessels become blocked and the blockage is not extensive.
- Bypass surgery may be used to bypass an artery that is blocked or severely narrowed as a result of vasculitis.
Surgery or angioplasty should not be performed during a flare/episode.
There is no way to prevent vasculitis or protect against it. Its causes are not well understood and its severity, duration and affected area/organ system vary greatly. Fortunately, with appropriate treatment most patients have a good overall outcome and lead functional and happy lives.
- It is essential that you avoid cigarette smoking to decrease complications from vasculitis.
- Ask your vascular surgeon how to lower your risk of infections.
- Take medications as prescribed.
- See your vascular surgeon as recommended.
