Catheter-directed thrombolytic therapy is a nonsurgical procedure that can be used to treat acute deep vein thrombosis (DVT). An acute DVT is a clot that typically occurs in your leg, thigh or pelvis but can travel. If a DVT travels to your lungs (referred to as a pulmonary embolism or PE), it can cause shortness of breath, chest pain, and lead to death.
This therapy may be an option to dissolve a DVT or PE more quickly than oral blood thinners.
- It should leave you with significantly less pain, swelling and other symptoms.
- If successful, it will also minimize damage inside the vein, which could lead to leaky valves and ongoing swelling, a condition known as chronic venous insufficiency or post-thrombotic syndrome.
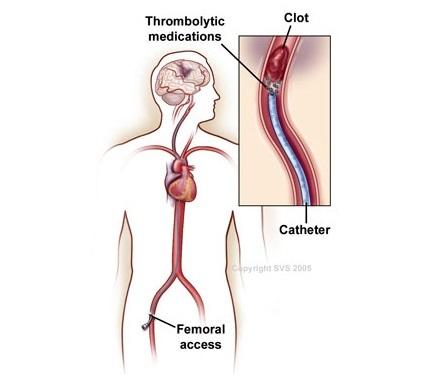
This therapy is performed in a catheterization lab or radiology suite. A team of doctors and nurses work together using a thin plastic tube (catheter) to deliver clot-dissolving medications called thrombolytics directly to the clot.
The Process
- You will be given medication for relaxation.
- After numbing your skin, a thin plastic tube is inserted into a vein, typically in your groin, neck or behind the knee.
- Medicine is infused through the tube and into the clot.
- If needed, a small machine is inserted through the tube to break up or suction the clot.
- Often a narrowed area in the vein is found, which may have led to the clot formation. This can be treated during the same therapy session with an angioplasty and/or a stent.
- An angioplasty is a treatment to widen the vein. After the blood clot is dissolved, a small device with an inflatable balloon is inserted and advanced through the tube. When the device reaches the spot where the vein has narrowed, the balloon is inflated and deflated several times, then removed.
- If the narrowing is severe, a stent may be placed inside the vein to keep it open. This usually takes additional time. A stent is a small metal-mesh tube. It is inserted and advanced through the tube to the spot where the vein has narrowed. The stent acts as a scaffold to support inside wall of the vein. It remains in the vein after the procedure.
- The catheter is removed at the end of the procedure.
- You may spend one or two days in the intensive care unit (ICU).
- You will be given additional medication to ensure the clot dissolves, usually in 12 to 14 hours.
- A compression stocking or sleeve will be placed on your leg.
- Your vascular surgeon will likely recommend you take an oral blood thinner for three to six months.
